Paresthesia
Definition of Paresthesia
Paresthesia comes from the Greek words, para (meaning abnormal) and aesthesia (meaning sensation).
This is the medical term used for the skin sensation that is described as tingling, tickling, pricking, burning, or numbing. It is also known as having the feeling of limb “falling asleep” or “pins and needles” [1]. This occurs without warning and is usually painless. It is more commonly felt in the arms, hands, feet, legs, and even on the other parts of the body [2].
Picture 1: Paresthesia sensation on hand
Source: andreemond.ca
Paresthesia Causes
Usually, paresthesia occurs due to the compression or damage of the nerves. It may also be manifested due to an underlying disease or injury that damages the nerves. [3]
Acute Paresthesia
Acute or transient paresthesias are the most frequent type of this condition. Usually, these occur at the hands or feet. These can be caused by either:
- Sustained pressure caused to the nerve: This pressure applied to the nerve will result to its inhibition or stimulation of its function. Removal of the applied pressure leads to gradual relief from paresthesia. Most common cases of paresthesia are brought by prolonged pressure that is applied to the nerves. Usually, this occurs after long periods of sleeping or sitting.
- Hyperventilation syndrome: This is characterized by mouth paresthesias and panic attacks.
Chronic Paresthesia
This kind of paresthesia is the kind that doesn’t go away. Chronic paresthesia is commonly known to be caused by an underlying traumatic nerve damage or neurologic disease. When a traumatic nerve damage or neurologic disease occurs, the pathways of the nerve transmission become impaired. Thus, sensation becomes affected. The specific causes of chronic paresthesias include:
1. Orthopedic causes
Some orthopedic conditions may cause damage or injury to the nerves. These include:
- Herniated disk
- Degenerative disk problem
- Bone fractures
- Tight, restrictive cast
- Osteoporosis
- Nerve pressure or entrapment like carpal tunnel syndrome
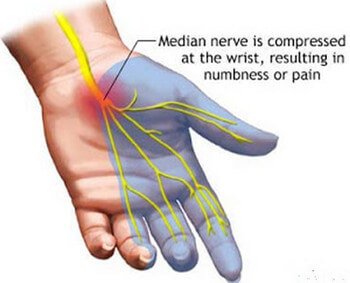
Picture 2: Paresthesia caused by Carpal Tunnel syndrome
Source: more-than-just-skin-deep.blogspot.com
- Neck or back injury
- Rheumatoid arthritis
2. Neurologic causes
- Tumors: Brain, spinal cord
- Inflammation: Encephalitis, Transverse myelitis, Neuritis
- Infection: Lyme disease, frostbite
- Demyelinating diseases: These affect the conduction of the nerve impulses. Some examples are Guillain Barre syndrome and multiple sclerosis.
- Herpes zoster disease: This causes the attacking of nerves which results to numbness.
- Autoimmune diseases: Lupus erythematosus, multiple sclerosis
- Nutrition-related: Alcohol abuse, Vitamin B12 deficiency, Diabetic neuropathy, malnutrition
- Arteriovenous malformation
- Stroke: Occurs most common in cases in which patient has Transient Ischemic Attack
- Poisoning: Heavy metal poisoning (lead, mercury)
- Peripheral neuropathy
- Migraine
3. Drug-related
- Benzodiazepine withdrawal
- Withdrawal from selective serotonin reuptake inhibitors (SSRIs)
- Beta-blockers
- Anticonvulsant drugs
- Lidocaine poisoning
4. Cardiovascular causes
Paresthesia caused by cardiovascular disorders occurs due to the impaired circulation in the extremities. The poor circulation in the extremities is caused by:
- Atherosclerosis: This is also known as the accumulation of plaque or fatty deposits within the walls of the arteries. As a result this leads to narrowing of the arteries.
- Peripheral vascular diseases: Also, develops from the narrowed arteries. Thus, resulting to poor circulation.
5. Metabolic disorders/ Electrolyte imbalance
- Hyperkalemia
- Hypomagnesemia
- Dehydration
- Diabetes (both hyperglycemia and hypoglycaemia)
- Hypoparathyroidism
- Hypothyroidism
6. Acroparesthesia
- This condition involves severe pain that is commonly felt at the extremities.
- Commonly caused by a condition called Fabry disease
7. Anesthesia
- Paresthesia induced by administration of anesthesia may either have temporary or permanent effects.
- Permanent paresthesia caused by anesthesia induction may have resulted from the extended numbness that occurred after local anesthesia administration.
- Other possible causes why anesthesia administration may have caused paresthesia are nerve sheath hemorrhage, nerve sheath trauma from injection, combination of anestheia and contaminated sterile solutions or alcohol, and the type of anesthesia used. [1, 2, 3, 4]
Paresthesia Symptoms
Paresthesia is known to be a symptom itself. Its occurrence may be caused by an underlying condition. Therefore, there are some symptoms that may accompany it. In most cases, the sensation becomes more pronounced upon applying pressure or tapping of the affected area.
Accompanying symptoms
- Pain
- Rash
- Sensitivity of the skin
- Muscle spasms
- Increased paresthesia felt during performance of a task, such as walking
- Frequent urination
- Anxiety
Serious accompanying symptoms
Paresthesia may be experienced together with other symptoms. This may be an indication of a life-threatening condition. When this occurs, immediate emergency care should be given. Here some of the serious symptoms that may occur with paresthesia:
- Loss of consciousness
- Confusion, dizziness
- Visual changes or visual loss
- Slurring of speech
- Paralysis, weakness
- Difficulty in breathing (Dyspnea)
- Inability to control bowel or bladder
- Walking difficulty [4, 5]
Paresthesia Treatment
The treatment of paresthesia is based on its determined underlying cause [5]. To determine the underlying cause of paresthesia, most doctors will order for nerve conduction studies and CT scan [1]. When the underlying cause is determined by the doctor, the treatment regimen can now be made. Also, the treatment will depend on the age of the individual and if there are any other existing diseases in the patient. This usually involves a plan which will address the underlying or associated cause [6].
Acute Paresthesia Treatment
1. Caused by pressure to the nerve
- Massaging, exercising or stretching the limbs affected

Picture 3: Stretching and exercising as relief for paresthesia
Source: healthclop.com
- Refrain from crossing legs
2. Anxiety/Panic attack
- If paresthesia is caused by anxiety attack, it will be gone when the episode ends.
Chronic Paresthesia Treatment
1. Tight Cast
- Cutting and opening of the cast to relieve pressure put on the nerves.
2. Cardiovascular Causes
- The focus of treatment in paresthesia caused by cardiovascular diseases would be controlling two factors. These are cholesterol levels and blood pressure.
3. Diabetic neuropathy
- Regular monitoring which involves controlling of the blood sugar levels
- Medications
- Diet appropriate for people with diabetes
3. Vitamin B12 deficiency
- Nutritional therapy (B complex supplements)
4. Medications for specific conditions
- Immunosuppressants such as prednisone
- Anticonvulsants like Gabapentin
- Antiviral medications for paresthesia caused by shingles
- Intravenous gamma globulin (IVIG)
5. Topical creams
These are given as a palliative treatment. Usually, these topical creams can cause numbing to relieve the sensation of paresthesia. These include:
- Lidocaine creams
- Prilocaine creams
6. Other forms of treatment for chronic causes of paresthesia are:
- Surgical interventions
- Physical and occupational therapy: Involves helping the patient perform activities of daily living (ADLs), use of assistive/orthopaedic devices.
- Changes in lifestyle and diet: includes refraining from alcohol consumption and intake of vitamin supplements
Alternative treatment
- Acupuncture: Believed to relieve paresthesia
- Self-massage: Ideally done with aromatic oils.
- Application of capsaicin-containing ointments also helps in resolving paresthesia.
- Stress management and adequate hours of sleep
- Exercise regimen
- Wearing appropriate and loose-fitting shoes and clothes. [5, 6, 7, 8]
References:
- http://en.wikipedia.org/wiki/Paresthesia
- http://www.ninds.nih.gov/disorders/paresthesia/paresthesia.htm
- http://neurology.about.com/b/2012/04/16/what-is-paresthesia.htm
- http://ezinearticles.com/?What-Is-Paresthesia?&id=6690912
- http://www.localhealth.com/article/paresthesia/causes
- http://www.disabled-world.com/health/neurology/paresthesia.php
- http://byebyedoctor.com/paresthesia/
- http://www.healthclop.com/different-causes-and-treatments-of-paresthesia/
Published by Dr. Raj MD under Diseases and Conditions.
Article was last reviewed on August 6th, 2018.

